Breaking Down Current Research: Cyclic Progesterone and Spironolactone Treatment for Polycystic Ovary Syndrome - A Feasibility Study by Kaitlin Nelson (MSc)
By: Sofia R.M. Jacome
Introduction
In a perfect world, every condition and disease would have a simple, effective, one-pill solution. However, underfunding in female reproductive health issues like polycystic ovary syndrome (PCOS) is common, despite the prevalence, economic burden, comorbidities and negative impact on quality of life.1 This underfunding prevents us from determining the best and most effective way of treating and managing conditions like PCOS.
Currently, most treatments aimed towards the management of PCOS are not treating the root cause of the condition itself, instead working to manage the symptoms associated with the condition. Common treatments include a combination of birth control pills to regulate the menstrual cycle, lifestyle modifications to improve things like cholesterol levels, and metformin to improve the body's inability to respond to insulin.2 While physical symptoms are the focus of treatment, for many living with PCOS, the condition also greatly affects their mental health.3 In addition to physical symptoms, this clinical trial also examines a treatment's effect on an individual's mental health.2
This pilot study, led by Kaitlin Nelson (MSc) and Dr. Jerilynn Prior, aimed to evaluate the efficacy of using a progesterone hormone treatment in combination with spironolactone, a medication that blocks male hormones like testosterone2,4. As of January 2025, very few studies, including this one, have examined the use of cyclic progesterone treatment for the management of PCOS.
Cyclic Progesterone Treatment
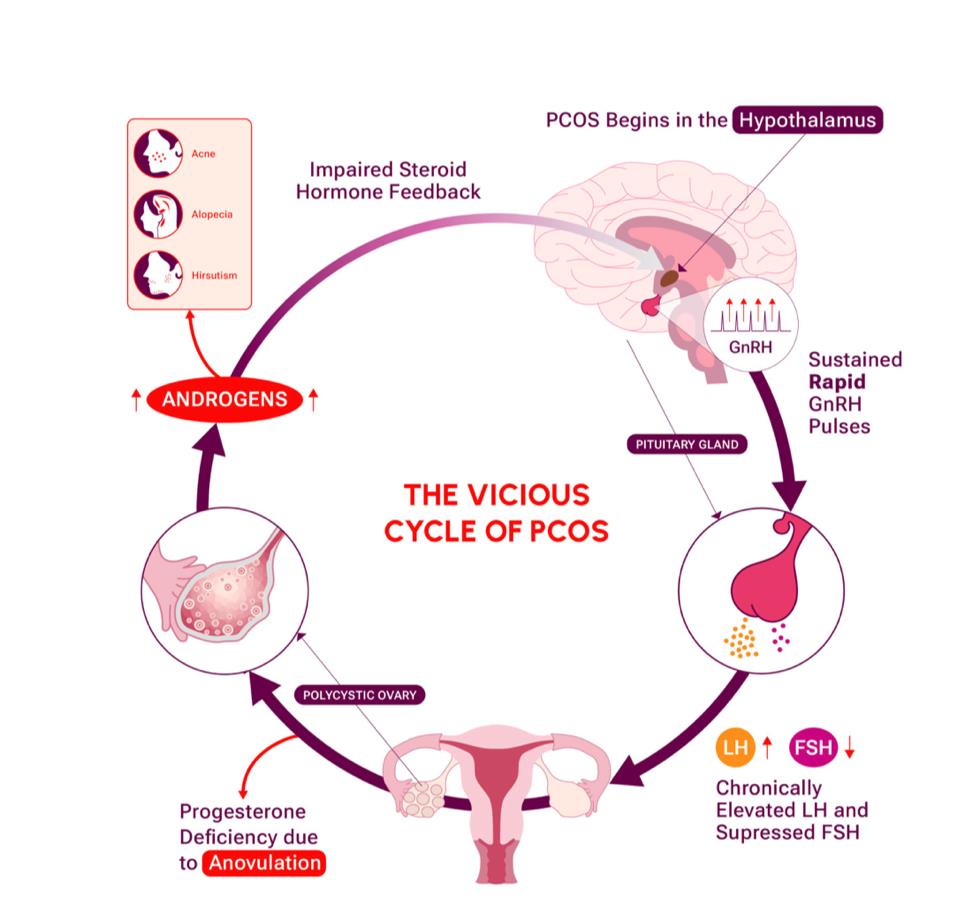
PCOS operates in a "feedback loop," a situation that can be described as having a certain hormone that impacts other hormones in a chain reaction, where the end of the chain further impacts the first hormone. This feedback continues in a cycle, and treatments must function to break this chain to improve symptoms.
In the PCOS feedback loop, a hormone called Gonadotropin-releasing hormone (GnRH) is released at an irregularly high frequency, which causes Luteinizing hormone (LH) to also be released at a high frequency.2Normally, LH works to develop the egg that will eventually be released during ovulation.5 While a spike in LH is normal just before an egg is released, the high frequency seen in PCOS leads to hormonal disruptions, including high testosterone levels, high estrogen levels, and low Follicle-stimulating hormone (FSH), leading to irregular menstrual cycles.2 Additionally, the high testosterone levels lead to symptoms we commonly associate with PCOS: alopecia, acne, and facial/body hair growth, as well as insulin resistance, reduced fertility, and increased cancer risks.2 The dysregulation of LH also impacts progesterone levels, a hormone necessary for preparing the uterus for pregnancy and regulation of the menstrual cycle by lowering LH levels in preparation for having a period.6 Since progesterone levels are too low in PCOS, the release of GnRH in the brain is not slowed down, leading us to the beginning of the cycle once again.7
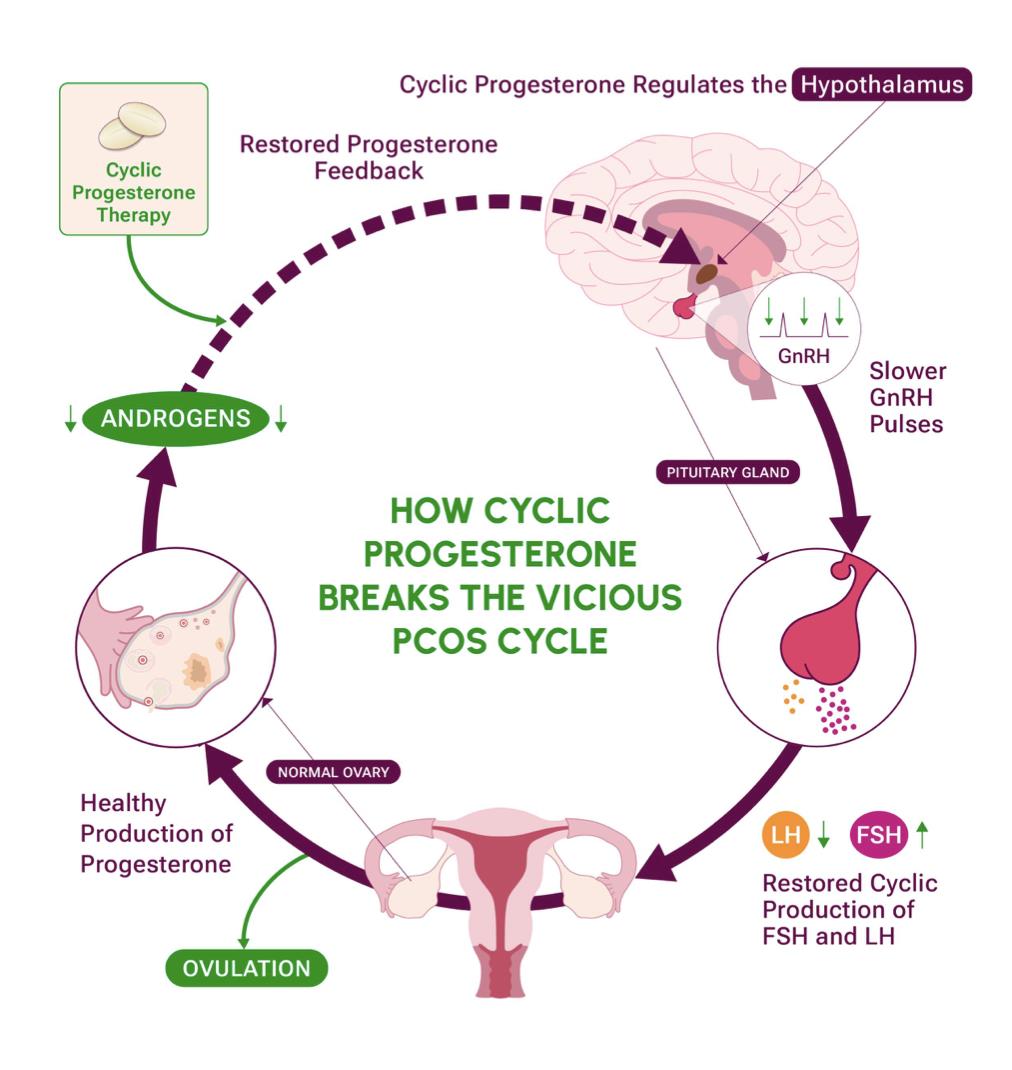
The reasoning behind the study was that since progesterone plays a role in slowing GnRH and, by extension, LH pulses, it could be used as a treatment to break the chain and restore a normal hormonal cycle.2 The progesterone is implemented in a "cyclic" manner, where instead of taking the pill every day, it is taken in the second half of the menstrual cycle (approximately days 14-28) to mimic the body's natural progesterone levels.8 This study is unique in also incorporating spironolactone, a diuretic "water pill" that is sometimes prescribed off-label to block male hormones like testosterone.9 This medication was implemented into the study for two reasons. The first is to block excessive testosterone levels that lead to unwanted facial hair, acne, and ovarian dysfunction.2 The second reason was that since high testosterone can impair the cyclic progesterone's ability to slow GnRH pulses, it could reduce the efficacy of the treatment; therefore Spironolactone was used to reduce these levels.2
Aim of the Study
The study aimed to evaluate the effectiveness of 6 months of cyclic progesterone therapy in combination with spironolactone in improving quality of life for individuals living with PCOS.2 The study followed participants' quality of life, which included 5 domains: emotions, body hair, weight, infertility, and menstruation.2 Additionally, hormone levels, acne, and sleep quality were assessed.2 This study followed a cohort of 26 individuals diagnosed with PCOS for 6 months.2
Results
The study found that this treatment enhanced overall quality of life in all 5 domains (emotions, body hair, weight, infertility, and menstruation) and alleviated PCOS symptoms.2Improvements were found in sleep quality and acne severity.2 Participant's testosterone and LH levels showed a statistically insignificant decrease; however, the average testosterone levels decreased to a range that is expected in individuals without PCOS, suggesting that this treatment was able to break the feedback loop that produced symptoms of high androgens.2 Additionally, the participants reported that they preferred this combined treatment instead of oral contraceptives.2
Study Limits
The researchers noted that this study was limited by its small size, only involving 26 individuals.2 Since the same dose of spironolactone was used for everyone, individuals with lower BMIs found this dose too high, and side effects may have contributed to participant drop out.2 Additionally, each participant was fixed to a 28-day cycle, taking progesterone for the last 14 days, instead of personalizing the therapy to each individual and their natural cycle.2
Why is this important?
This study was only the second to explore the use of cyclic progesterone therapy for treating PCOS.2 Studies involving combined oral contraceptives found that birth control was unable to break the feedback loop the same way cyclic progesterone is.2 This study demonstrates a need for exploration into better, more effective treatments for PCOS, specifically treatments that are able to break the chain of dysfunction and fix the underlying issues, instead of treating individual symptoms. Continuing research into this treatment and transforming it into a personalized therapy with specific doses and cycles for each individual could also allow it to be a highly effective, tailored treatment for many with PCOS. With so few treatments currently available, it is essential for researchers like Kaitlin Nelson to seek out new, improved therapies to enhance health care for managing and treating PCOS.
Bibliography
- Brakta S, Lizneva D, Mykhalchenko K, Imam A, Walker W, Diamond MP, et al. Perspectives on polycystic ovary syndrome: Is polycystic ovary syndrome research underfunded? The Journal of Clinical Endocrinology & Metabolism [Internet]. 2017 Sep 19;102(12):4421-7. Available from: https://doi.org/10.1210/jc.2017-01415
- Nelson K. Phase II 6-month cyclic progesterone/spironolactone pilot therapy trial in polycystic ovary syndrome - a pre-post one-arm feasibility study. Open Collections [Internet]. 2025 Jan 1; Available from: https://doi.org/10.14288/1.0447691
- Dewani D, Karwade P, Mahajan KS. The Invisible Struggle: The Psychosocial aspects of Polycystic Ovary Syndrome. Cureus [Internet]. 2023 Dec 30;15(12):e51321. Available from: https://doi.org/10.7759/cureus.51321
- HealthMatch staff, HealthMatch Pty Ltd. How does spironolactone help in treating PCOS? [Internet]. HealthMatch. 2022. Available from: https://healthmatch.io/pcos/spironolactone-for-pcos
- Cleveland Clinic. Luteinizing hormone [Internet]. Cleveland Clinic. 2025. Available from: https://my.clevelandclinic.org/health/body/22255-luteinizing-hormone
- Cleveland Clinic. Progesterone [Internet]. Cleveland Clinic. 2022. Available from: https://my.clevelandclinic.org/health/body/24562-progesterone
- Bashour NM, Wray S. Progesterone directly and rapidly inhibits GNRH neuronal activity via progesterone receptor membrane component 1. Endocrinology [Internet]. 2012 Sep 1;153(9):4457-69. Available from: https://doi.org/10.1210/en.2012-1122
- The Centre for Menstrual Cycle and Ovulation Research (CeMCOR). Cyclic Progesterone Therapy - CEMCOR [Internet]. CeMCOR. 2025. Available from: https://cemcor.ubc.ca/resources/cyclic-progesterone-therapy/
- Spironolactone (oral route) [Internet]. Mayo Clinic. 2026. Available from: https://www.mayoclinic.org/drugs-supplements/spironolactone-oralroute/description/drg-20071534